| Fig. 1. A normal complement of adult teeth (source: internet) |  |
Symptoms, Signs, and Consequences of Bruxism
Sleep bruxism often exerts remarkably powerful forces on teeth, gums, and joints. One estimate puts it at three times the forces generated during chewing (Castaneda, 1992, p. 46), while another puts it at ten times—powerful enough to crack a walnut.
Why are these forces so high? First, the bruxing activity is not under control of the conscious, rational, brain, which might have moderated or prevented the act from occurring. Second, when one eats, the chewing force is applied in part to the food, not to the teeth; but when one bruxes, the entire force is applied directly to the teeth.
While not a life-threatening condition, chronic bruxism often impairs the quality of life of affected individuals. Some suspected symptoms and consequences of this habit are listed below:
I. Chronic bruxism may lead to sensitive, worn-out, decayed, fractured, loose, or missing teeth (McGuire and Nunn, 1996).
| Fig. 1. A normal complement of adult teeth (source: internet) |  |
Grinding or clenching break down the enamel, sometimes, in long-term bruxers, reducing teeth to stumps. Instead of a white enamel cover, one often sees the more yellowish and softer dentin. The back teeth of some chronic bruxers often lose their cusps and natural contours, appearing instead flat, as if they had been worked over with a file or sandpaper. When anterior teeth are affected, their biting surfaces are damaged. As well, the absence of enamel makes it easier for bacteria to penetrate the softer part of the teeth and produce cavities. With time, the condition may lead to bridges, crowns, root canals, implants, partial dentures, and even complete dentures.
As long as bruxism continues, the situation keeps getting worse. Thus, "by 40 or 50 years of age, most bruxers . . . have worn their teeth to the degree that extensive tooth restorations must be performed" (Christensen, 1999). For example, implant complications are more likely in people who habitually clench or grind their teeth (Perl, 1994, Nishimura et al., 1997). In one study, more than 75% of observed implant fractures occurred in patients with signs and histories of chronic bruxism. Hence, in cases of untreatable severe bruxism, the use of implants is strongly counterindicated (Rangert et al., 1995.; reviewed by Nishimura et al., 1997).
II. Long-term bruxism often causes changes of appearance, in at least three different ways.
To begin with, damaged, worn-out teeth are not as appealing as healthy teeth.
Second, as the teeth wear out, they become shorter. As a result, when the mouth is closed, the upper and lower jaws are nearer than they used to be, and so are the nose and chin. The skin now may bag below the eyes and curl around the lips, causing the lips to seemingly disappear (Schlott, 1997). The chin recedes, and the person looks comparatively old.
| Fig. 2. The young man (left frame) has normal teeth. By middle age (middle frame), bruxism flattened this man’s teeth and changed his appearance somewhat. By old age (right frame), the change is even more remarkable (Source: Gelb, 1994, p. 227). |  |
Third, bruxism involves excessive muscle use, leading to a build-up or enlargement (hypertrophy) of facial muscles, especially those of the jowl (where the masseter muscle--the muscle that raises the lower jaw and enables closing the jaws--is located). In long-term bruxers, this build-up may lead to a characteristic, square-jaw, appearance. Some patients resort to removing part of the masseter muscle by surgery or injections of toxic materials to reduce muscle size and thus partially regain their former, more aesthetically pleasing, looks (Mandel & Tharakan, 1999; Rijsdijk et al. 1998).
| Fig. 3. Facial appearance of a 13-year-old bruxer with left masseteric hypertrophy (arrow on right). Source: Mandel & Tharakan, 1999. | 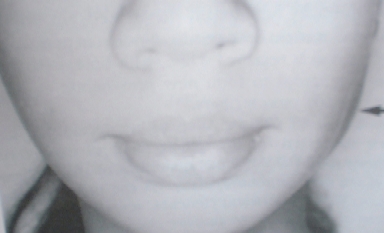 |
| Fig. 4. Masseter muscle. Source: Life Art |  |
III. Long-term bruxers sometimes experience jaw tenderness; jaw pain; fatigue of facial muscles; headaches; neck aches; tinnitus (ear ringing; Fernandes et al., 2014); earaches; and hearing loss (Bubon, 1995). Our body is not built to sustain, night in and night out, the tremendous pressures of bruxing. The teeth, as we have seen, are affected, but in some cases other parts of the head suffer too. We need to note, in passing, that such aches and pains are a functional, healthy, response. It’s the body's way of sending a message: stop bruxing, or else!
IV. Another example of this spiral involves the occasional inflammation and blockage of some salivary glands. As before, the causal sequence is pretty simple. Like body building, bruxism involves muscle overuse. In this case, the masseter muscles become disproportionately overdeveloped and block the opening of the nearby parotid glands. They thus interfere with the flow of saliva into the mouth, causing the saliva to accumulate in the glands. This in turn may lead to periodical swelling, pain, inflammation, and abnormal dryness of the mouth (Mehta, 1992, p.134) .
V. Bruxism may also damage the temporomandibular joints (TMJs). Bruxism is therefore believed by most researchers (but not all, cf. Lobbezoo & Lavigne, 1997) to be one of the leading causes of temporomandibular disorders (TMDs) (Glaros, Tabacchi, & Glass, 1998; Israel et al., 1999; Yustin et al., 1993).
| Fig. 5. The temporomandibular Joint (TMJ). Source: Internet |  |
To be sure, besides bruxism, TMDs may be caused by such things as whiplash, a hard blow to the chin, malocclusion, nearby tumors, orthodontic treatment, arthritis, long-term scuba diving, or prolonged violin playing. But the important point here is that chronic bruxism may induce TMDs, and that TMDs can be unpleasant. Often, the first warning signs of TMDs are TMJ discomfort or pain, soreness of jaws and muscles, clicking or popping sounds when opening the jaws or while chewing, and difficulties in fully opening the mouth. If bruxism continues at this point, these symptoms become more severe. TMDs are often associated with chronic pain which may last months or years. A sufferer may wake up, for example, totally unable to open the mouth. Or the jaw may suddenly lock or dislocate during chewing. Eventually, a difficult surgery of uncertain efficacy may be required.
It is worth remembering that a "TM disorder, although not being life threatening, is certainly life altering." It can, in fact, "devastate its victim" (Goldman, 1992, p. 191). First, patients must contend with chronic pain and other symptoms. Second, often, there is much anguish and humiliation before the condition is correctly diagnosed. Indeed, "the average TM disorder patient has been seen by at least seven physicians, dentists, psychologists, or other health professionals. Of these patients, 7 out of ten have been incompletely diagnosed or misdiagnosed" (Goldman, 1992, p. 215). Third, "it is unrealistic to expect" a cure for TMDs. "At best, we are only managing signs and symptoms to the best of our ability within the framework of the patient's ability to cope with the disorder" (Pertes & Attansio, 1992, p. 146). The best thing we can do for our bruxing patients, then, is to help them control bruxism and thereby minimize the chances of temporomandibular complications.
Conversely, when TMDs are traceable to bruxism, it is more or less useless to treat these disorders without addressing their underlying cause: "Surgical procedures that alter anatomic relationships without addressing factors contributing to pathogenesis may be more prone to failure and recurrence of [TMD] symptoms. It is clear that excessive loading on articular tissues is one of the causative factors that must be identified and addressed by all clinicians treating patients with TMJ pathology" (Israel et. al, 1999, p. 1039).
VI. Dental fillings often contain solid mercury. Mercury, in turn, is not entirely safe. Right now, the consensus of the dental community in the USA is that the advantages of using mercury outweigh the comparatively small risks. According to the American Dental Association, for example, "there is insufficient evidence to justify claims that mercury from dental amalgams has an adverse effect on the health of patients" (cited in Scully and Cawson, 1993, p. 377). Others claim that mercury does have adverse effects and it ought not to be used. But, regardless of the outcome of this controversy, In bruxers, the situation is a bit more complicated, for there is some evidence of higher levels of mercury in the blood of some bruxers with mercury fillings (Isacsson et al., 1997).
VII. Malocclusion, or bad bite, is more common among bruxers than in the general population. To be sure, misaligned teeth may serve as the cause of bruxism, not as its consequence. But bruxism may often involve more pressure on one side of the mouth than on the other, thereby causing malocclusion. As well, as the teeth wear out and the distance between the upper and lower jaws decreases, overclosure may develop--when bruxers close their mouth the front upper teeth do not meet the front lower teeth, but get in front of them.
VIII. Clenchers, as we have seen, destroy their teeth silently, and their habit therefore does not directly impinge on members of their household. Grinders find themselves in a more uncomfortable position, for many people find the grinding sound unpleasant, irritating, or disturbing (Blount et al., 1982; Watson, 1993). It may wake up light sleepers, for instance, and keep them awake for a long time.
Conclusion. The picture that emerges, then, is of a habit that is not life-threatening in any way. Moreover, in its initial stages, because bruxism only involves minor symptoms and inconveniences, it is often ignored by both patients and clinicians. At a certain point, however, the symptoms begin to noticeably affect one’s quality of life. It is typically at this point that a patient starts looking for a cure. This delay is unfortunate, for by then the habit is ingrained and has already brought about irreversible losses.
REFERENCES
Blount, R. L., Drabman, N. W., Wilson, W., & Stewart, D. (1982). Reducing severe diurnal bruxism in two profoundly retarded females. Journal of Applied Behavior Analysis, 15, 565-71.
Bubon, M. S. (1995). Documented instance of restored conductive hearing loss. Functional Orthodontist, 12, 26-9.
Castaneda, R. (1992). Occlusion. In A. S. Kaplan & L. A. Assael (Eds). Temporomandibular Disorders (pp. 40-49). Philadelphia: Saunders.
Christensen, G. J. (1999). Destruction of human teeth. Journal of the American Dental Association, 130, 1229-30.
Fernandes, G. et al. (2014). Association between painful temporomandibular disorders, sleep bruxism and tinnitus. Braz Oral Res. 9;28(1):1-7.
Glaros, A. G. Tabacchi, K. N., & Glass, E. G. (1998). Effect of parafunctional clenching on TMD pain. Journal of Orofacial Pain, 12, 145-152.
Gelb, H. (1994, Ed). New concepts in Craniomandibular and Chronic Pain Management. Mosby-Wolfe.
Goldman, J. R. (1992). Soft Tissue Trauma. In A. S. Kaplan & L. A. Assael (Eds). Temporomandibular Disorders (pp. 191-223). Philadelphia: Saunders.
Isacsson, G., Barregard, L, Selden, A., & Bodin, L. (1997). Impact of nocturnal bruxism on mercury uptake from dental amalgams. European Journal of Oral Sciences, 105, 251-257.
Israel, H. A., Diamond, B., Saed-Nejad, F., & Ratcliffe, A. (1999). The relationship between parafunctional masticatory activity and arthroscopically diagnosed temporomandibular joint pathology. Journal of Oral and Maxillofacial Surgery, 57 (9), 1034-9.
Lobbezoo, F., & Lavigne, G. J. (1997). Do bruxism and temporomandibular disorders have a cause-and-effect relationship? *Journal of Orofacial Pain, 11 (1), 15-23
Mandel, L. & Tharakan, M. (1999). Treatment of unilateral masseteric hypertrophy with botulinum toxin: case report. Journal of Oral and Maxillofacial Surgery, 57, 1017-1019.
Mcguire, M. K., & Nunn, M. E. (1996). Prognosis versus actual outcome: III. The effectiveness of clinical parameters in accurately predicting tooth survival. Journal of Periodontology, 67, 666-674.
Mehta, Noshir (1992). Muscular Disorders. In Kaplan, A. S. & Assael, L. A. Temporomandibular Disorders. Philadelphia: Saunders, pp. 118-141.
Nishimura,, R. D., Beumer, J, 3rd, Perri, G. R., Davodi, A. (1997). Implants in the partially edentulous patient: restorative considerations. CDA Journal, 25, 867-871.
Perl, M. L. (1994). Parafunctional habits, nightguards, and root form implants. Implant Dentistry, 3, 261-3.
Pertes, Richard A. & Attanasio. Ronald (1992). Internal Derangements. In Kaplan, A. S. and Assael, L. A. Temporomandibular Disorders. Philadelphia: Saunders, pp. 142-164.
Rangert, B., et al. (1995). Bending overload and implant fracture. A retrospective clinical analysis. International Journal of Oral Maxillofacial Implants, 10, 326-34.
Rijsdijk, B. A., Van Es R. J., Zonneveld, F. W., Steenks, M. H., & Koole, R. (1998). Botulinum toxin type A treatment of cosmetically disturbing masseteric hypertrophy. Nederlands Tijdschrift voor Geneeskunde, 142, 529-32.
Schlott, W. J.(1997). Midface collapse: an overlooked disease. Dentistry Today, 16(9):54-7
Scully, Crispian & Cawson, Roderick A. (1993). Medical Problems in Dentistry, 3rd edition. Oxford: Wright.
Watson, T. S. (1993). Effectiveness of arousal and arousal plus overcorrection to reduce nocturnal bruxism. Journal of Behavior Therapy and Experimental Psychiatry 24, 181-185.
Yustin, D., Neff, P., Rieger, M. R., & Hurst, T. (1993). Characterization of 86 bruxing patients and long-term study of their management with occlusal devices and other forms of therapy. Journal of Orofacial Pain 7: 54-60.